Seriously ill Doncaster toddler is given UK's first ever pig skin transplant


Little Eve Phillipson underwent the surgery to create her an artificial diaphragm with medics carefully inserting the animal skin inside her body after she was born with a life threatening condition.
The two-year-old from is now being held up as 'a little ray of hope’ for families nationwide thanks to the operation at Sheffield Children’s Hospital.


Advertisement
Hide AdAdvertisement
Hide AdEve was diagnosed with Congenital Diaphragmatic Hernia (CDH) while still in the womb. The condition, which affects one in every 10,000 new-born babies, occurs when there is a hole in the muscle that separates the chest from the stomach.
This causes the bowel and other organs to enter the chest and squash the developing lungs.
Mum Rebecca, 38, said: “We went to our 12 week scan and she had more fluid than normal on the back of her neck, so they scanned Eve again at 15 weeks and found the CDH”.
Eve’s case was particularly severe. While the majority of CDH sufferers have small holes in the diaphragm, Eve’s was missing completely and she required immediate life support when she was born.


Advertisement
Hide AdAdvertisement
Hide AdSurgical teams at Sheffield and Leicester operated on Eve to replace the missing diaphragm, with the first surgery taking place when she was just one week old.
The initial procedure involved using a Gortex patch, similar to the material found in raincoats, while the second repair combined nylon into the patch. Unfortunately, neither artificial implant held and Eve’s health started to decline as she grew older:
“By her second birthday we were concerned that if we didn’t go for the ground-breaking surgery to create a natural diaphragm, we might lose her," Rebecca explained.
The five-hour procedure saw two of the three muscles in Eve’s abdominal wall being delicately turned to create a natural diaphragm. Medically-sterilised pig skin, known as Strattice, was then used to reinforce the weakness in her abdominal wall.

Advertisement
Hide AdAdvertisement
Hide AdThe operation was carried out by Sean Marven, Consultant Paediatric Surgeon at Sheffield Children’s NHS Foundation Trust, who recalls the dilemma of timing the procedure.
“It was a very difficult decision. We knew the longer we waited, the more perilous the procedure may be. The surgery was complex and required a great deal of skill and concentration, particularly as it had never been performed in the UK before. Thankfully it went well and Eve continues to grow stronger."
In addition to the innovative surgical progress, The Children’s Hospital Charity is also funding research to improve the information provided to surgeons and parents during pregnancy where CDH is suspected in the unborn baby.
The worrying time waiting for birth is something Eve’s mum was all too aware of.


Advertisement
Hide AdAdvertisement
Hide AdShe said: “It was quite overwhelming. We were told she had a 50:50 chance of survival and we didn’t know the extent of the damage until she was born. It was an emotional rollercoaster and an incredibly anxious time."
The research project uses an MRI scan taken at the same time as a routine pregnancy ultrasound to make 3D animations and models of the unborn baby and their individual CDH.
This helps the surgeons see the extent of the damage and the displaced organs, allowing them to choose the best type of operation and material to treat the patient. Crucially, the models and images would also be provided to parents, helping to ease their anxiety.
The study forms part of The Children’s Hospital Charity’s annual commitment to spend up to £250,000 on research into the prevention and cure of childhood illnesses.
Advertisement
Hide AdAdvertisement
Hide AdThe lead researcher, Dr Elspeth H Whitby, Senior Lecturer at the University of Sheffield said: “The project wouldn’t have been possible without funding from The Children’s Hospital Charity. The research will help families and patients at Sheffield Children’s Hospital, but it will also benefit any family dealing with CDH in Yorkshire and could be implemented nationwide if successful”.
The Children’s Hospital Charity’s Director David Vernon-Edwards added: “As a charity we are very proud to play an important role in ensuring that innovative research continues to be funded, helping children to get better and lead full lives. Eve’s incredible resilience is an inspiration to us all”.


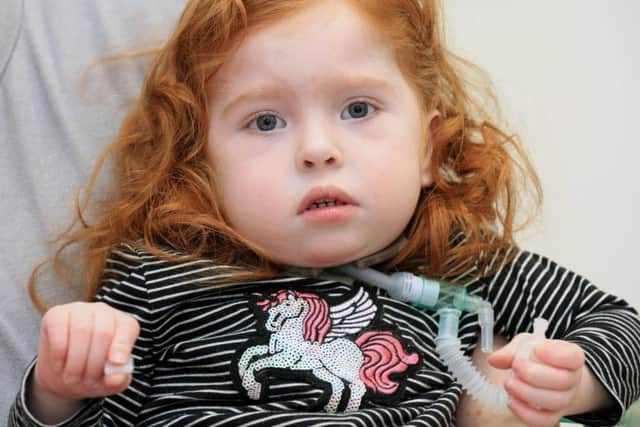
Eve continues to require 24/7 ventilation and oxygen due to the initial damage caused by her condition, which resulted in the collapse of her left lung. Her family are hopeful that she will be able to live without the support in the future.
Nevertheless it’s clear that the youngster today lives as happy a life as any two year-old in spite of the challenges she faces.
Advertisement
Hide AdAdvertisement
Hide Ad“She smiles, she plays, she’s mischievous, she’s funny; what more can you ask for than that. It will be nice when we get her off the ventilator and off oxygen, but we’ll get there when we get there” added Rebecca.
“If other families are going through a dark time, Eve can be a little ray of hope for them. Sometimes even the worst cases can turn out well”.
To find out more about this research project and others funded by The Children’s Hospital Charity, visit www.tchc.org.uk